Closure of left atrial appendage (LAA)
What is it?
What is it?The left atrial appendage is a small pouch in the wall of the left atrium that has no essential function. During heart rhythm disturbances such as atrial fibrillation, blood clots may form here. These blood clots may be dangerous and, for instance, cause stroke. The formation of blood clots therefore must be avoided. This can be done by taking blood thinners or alternatively, if this is not possible or is insufficiently effective, surgery may be opted for.
What is the process?
What is the process?Preparation
You will be admitted to the Cardiology Day Hospital. You need to have fasted for eight hours before admission. Medication may be taken as agreed with the physician.
You will be given a surgical gown to wear and the nurse will place an IV line in your arm to administer medication later. Approximately one hour before the procedure, you will be given a 300-mg dose of Plavix and preventative antibiotics through the IV drip. Some patients are allergic to certain types of antibiotics, so they must inform the nurse of this on admission Blood samples will be collected, an electrocardiogram will be performed and if necessary, an X-ray will be taken of the lungs.
The procedure is performed under general anaesthetic in the cardiac catheterisation room.
The procedure
You lay down on the examination table. Electrodes are placed to monitor your heart rhythm. A blood pressure monitor will be placed around your arm and a clip will be placed on your fingertip to monitor oxygen levels during the procedure. The anaesthetist will prepare you for and then administer the anaesthesia.
Once you are asleep, a puncture will be made in the groin area. A long, flexible tube is inserted into a vein in the groin and threaded up to the right atrium of the heart. A catheter can be introduced through a small puncture in the partition between the atria into the left atrium, up to the left atrial appendage.
Through this catheter, a folded plug, or ‘umbrella’, can be brought up into the left atrial appendage. This plug, or umbrella, unfolds so that the appendage is fully closed. The small opening in the partition between the atria, caused by the puncture, will close spontaneously after a few weeks to months. The entire procedure is performed with the support of oesophageal ultrasound.
Aftercare
Manual pressure will be applied to the groin and a pressure bandage will be fitted. For that reason, you will be need to observe bed rest for 12 hours. In the hours following the procedure, the nurse will check your blood pressure, pulse, the puncture site and any potential discomforts.
Discharge is scheduled for the day after the procedure. On that day, an echocardiography and an X-ray will be performed and blood samples will be taken. It is recommended to arrange for transport on discharge and to avoid driving yourself.
Contact your GP in case of the following symptoms:
- Fever (from 38 °C)
- Shortness of breath
- Heart palpitations
- Dizziness
- Bleeding
- Persistent pain or swelling of the groin
- Wound leakage
- Redness and/or warm sensation in the groin
- Pain or numbness of the legs when walking
- Skin rash
The procedure is generally estimated to require five days off work, but this depends on the degree of physical effort involved in the work. You will need to take anticoagulants (75 mg of Clopidogrel in combination with 80 mg of Asaflow) for two months. Other blood thinners may be stopped.
Important: during the first six months after the procedure, you will always need to take antibiotics (prophylaxis) in the event of bloody, non-sterile procedures.
What are the risks?
What are the risks?Complications are extremely rare but may have serious consequences. The following are possible complications:
- cardiac tamponade
- air embolism
- infection
- migration of the umbrella-shaped device
Results
ResultsOnce the plug (or umbrella) is in place, checks are performed to verify that the left atrial appendage is fully closed. To this end, you will be injected with a contrast agent. Some patients are allergic to contrast agents and must inform the nurse of this on admission.
Leaflet
LeafletSee the leaflet below for more information.
Only available in Dutch:
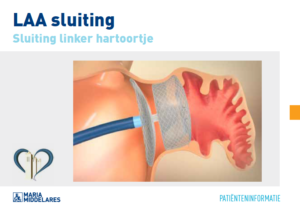
Sluiten linker hartoortje
DownloadCentres and specialist areas
Centres and specialist areas
Latest publication date: 16/05/2024
Supervising author: Dr Provenier Frank



