Unblocking or widening of coronary arteries
What is it?
What is it?By threading catheters through the arteries to the heart, the physician can view the coronary arteries using a contrast agent and X-rays. If diagnostic cardiac catheterisation demonstrates major constrictions, the cardiologist can unblock the coronary artery with a balloon or stent. This is generally done as part of the same procedure. An acute heart attack due to a blocked coronary artery requires unblocking as soon as possible. The longer the blood circulation is interrupted, the higher the risk of irreversible damage to heart muscle tissue as a result of oxygen deprivation.
What is the process?
What is the process?Preparation
If you are admitted with acute heart symptoms, you will be referred for cardiac catheterisation as soon as possible. To this end, the cardiologist and the nursing team provide 24/7 on-call cover.
If your symptoms are not acute, the procedure is performed by appointment. You will be admitted to the Cardiology Day Hospital on the scheduled date. You need to have fasted before and on the day of your admission. This means only clear liquids (e.g. only water, tea, and coffee) for a minimum of two hours beforehand. You may eat a light meal and consume dairy products no later than of six hours beforehand, and a normal meal no later than eight hours before admission. Your physician will tell you which medication you may take prior to the procedure.
If no recent laboratory results are available, blood samples will be taken. You will be given a surgical gown to wear. Shortly before the procedure, you can be provided with a tablet to help you relax. The nurse places an IV line in your arm for the administration of medication, should that be necessary.
Treatment
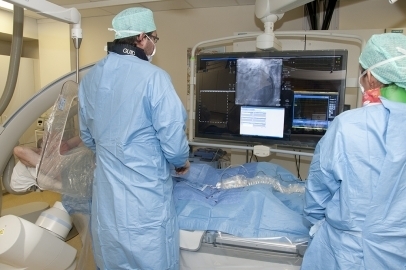
The procedure is performed in the cardiac catheterisation room where you take place on the treatment table. Adhesive electrodes are placed to monitor your heart rhythm. Under a local anaesthetic, a thin tube (≤ 2 mm) is placed in the artery in the groin, wrist or inside of the elbow. Through this tube, different catheters are threaded to near the heart to insert contrast agent directly into the coronary arteries. This contrast agent will be made visible on the screen using X-rays.
A very fine wire (± 0.3 mm) is inserted through and past the constriction in the coronary artery. Then, the constriction is eliminated through balloon dilatation or by placing a stent.
- Balloon dilatation: a balloon catheter is threaded over the wire up to the constriction. The balloon is then inflated to widen the constricted area.
- Stent placement: after the balloon dilatation, a second catheter with balloon and stent (metal spring) is inserted up to the constriction. When the balloon is inflated the stent unfolds and is pushed into the vessel wall.
Once the constriction is unblocked, the balloon is deflated and the catheter is removed. The stent remains in place. Once placed, a stent remains in place for the rest of your life and prevents the blood vessel from collapsing.
Aftercare
After coronary artery therapy, you will be kept under observation for 24 hours. The puncture site is checked regularly by the nurse of the ward you are staying in. The duration of the required bed rest mainly depends on the puncture site.
What are the risks?
What are the risks?- Contrast agent allergy: inform the cardiologist or nurse if you have an allergy to contrast agents containing iodine.
- Bleeding: blood loss may occur at the puncture site during, but also after the procedure. This risk varies greatly depending on the puncture site, but also depending on the degree of blood thinning. In rare cases, surgical repair of the blood vessel may be necessary.
- Embolism: in rare cases, a thrombus (a clot) can form on the catheter. This is prevented as much as possible by administering blood thinners during the procedure.
- Dissection: after balloon dilatation, a piece of the inner wall of the blood vessel can come loose. This is termed dissection and is treated with a stent.
- Perforation: in very rare cases, perforation of the treated blood vessel may occur, which results in blood loss outside the vessel.
- Tamponade: if perforation occurs, the bleeding in the sac around the heart may result in tamponade, which prevents the heart from pumping well. This fluid is drained as quickly as possible and the perforation is closed by using special stents.
- In some patients, a new constriction can develop over time (usually within the first six months) in the stent because of the scar tissue (i.e. in-stent restenosis). If this happens, a special type of stent (drug-eluting stent or DES) should be placed. A DES is treated with medication that inhibits the formation of scar tissue. Some patients are at increased risk of in-stent restenosis; therefore, the physician will place a DES straight away (e.g. for diabetic patients).
Leaflet
LeafletSee the leaflet below for more information.
Only available in Dutch:

Openen of dilateren van de kransslagaders
DownloadCentres and specialist areas
Centres and specialist areas
Latest publication date: 16/05/2024
Supervising author: Dr Provenier Frank



