Colonoscopy
What is it?
What is it?The colonoscopy is the most sophisticated procedure for bowel problems. It is a very safe procedure that is usually performed without any problems. Because of widely variable pain thresholds between individuals, we offer the option of having the procedure performed under anaesthesia, administered by an anaesthetist.
During the procedure, a flexible tube fitted with a video camera is inserted through the anus. The examination allows for the detection of inflammation, ulcers, polyps, malignant tumours and many other conditions at an early stage. Radiology examination (imaging) of the large intestine and scans (CT or MR) are also used to examine colon complaints, but do not provide the same precise information.
When?
When?The decision to perform a colonoscopy is taken by your GP or specialist after thorough examination of your symptims, clinical tests and possibly other, additional tests. If your physician recommends a colonoscopy and you decline, this may result in a delayed or mistaken diagnosis, with possible unpleasant consequences and therapy options that are not optimal.
Preparation
PreparationA coloscopy is preceded by thorough preparation, because the colon must be completely clean. This is because the view and assessment of the colon wall must not be hindered by the presence of stools.
If it is performed without adequate preparation, the examination is less reliable and abnormalities may be missed. A poorly prepared procedure is more difficult to perform and carries more risk.
You can read the guidelines for preparing for a colonoscopy with Moviprep or any of the other bowel preparations in the brochures located at the bottom of this page.
Process
ProcessView this video on the course of outpatient admissions for a colonoscopy:
Safety and hygiene
Safety and hygieneWe are an experienced and well-trained team, equipped with a modern infrastructure.
The anaesthetic is administered by an anaesthetist.
The procedure is performed in an endoscopy room that is equipped with all the necessary anaesthesia equipment and endoscopy instruments.
Before and after each test, each endoscope is thoroughly cleaned and disinfected in an automatic cleaning and disinfection machine in a controlled procedure. Our disinfection protocols meet European standards.
We use disposable materials for taking tissue samples (biopsy), injecting medication and removing polyps.
Possible complications
Possible complicationsIn principle, complications hardly ever occur. A very rare complication is perforation (i.e. tear) of the intestine. In that case, you will need urgent surgery. In rare cases, bleeding occurs after the removal of polyps. This may also require an urgent operation.
In rare cases, phlebitis can develop at the IV insertion site.
Things to consider
Things to considerDo not hesitate to ask for additional explanation should you have any doubts or queries. Inform us if:
- Pregnancy
- Allergy, sensitivity or intolerance (e.g. latex, Lidocaine)
- Clotting problems or use of blood thinners (e.g. Marevan, Sintrom, Marcoumar, Ticlid, Plavix, Pradaxa, Xarelto, Aspirin, etc.)
- Some patients who have an artificial valve or prosthetic require antibiotics before and after a procedure
- Epilepsy, diabetes, chronic heart, lung and kidney disorders: special attention to medication required
Leave removable dentures in your room. Damage to teeth (higher risk if teeth are in poor condition) cannot be ruled out during an endoscopy or anaesthesia.
Contact us if you have the following symptoms after the procedure:
- Persistent severe pain
- Fever
- Blood loss (red or black stools)
- Any concerning symptom
Postpolypectomy guidelines after a colonoscopy
Postpolypectomy guidelines after a colonoscopy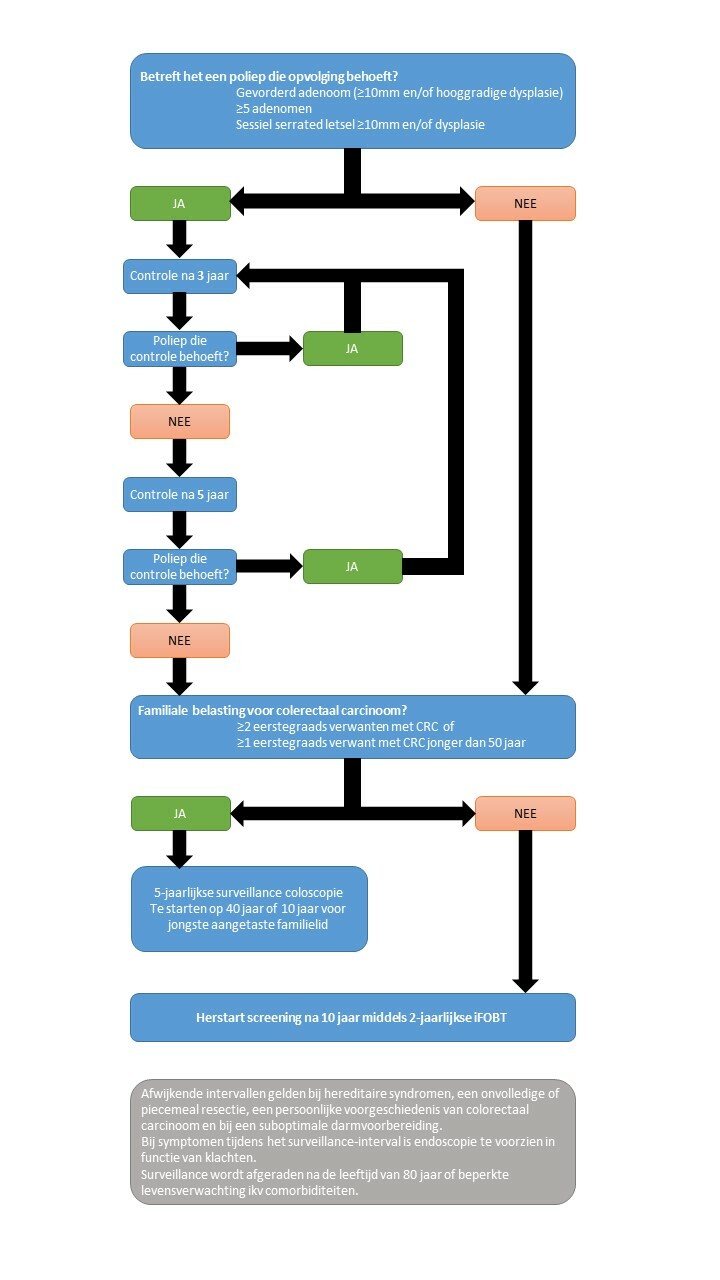
Leaflets
LeafletsOnly available in Dutch:

Coloscopie: voorbereiding met Moviprep
DownloadOnly available in Dutch:

Coloscopie: voorbereiding met Picoprep
DownloadOnly available in Dutch:

Coloscopie: voorbereiding met Plenvu
DownloadOnly available in Dutch:

Coloscopie: voorbereiding met Eziclen
DownloadOnly available in Dutch:

Coloscopie: voorbereiding met Eziclen bij dialysepatiënten
DownloadOnly available in Dutch:

Coloscopie: voorbereiding met Citrafleet
DownloadCost estimate
Cost estimateCentres and specialist areas
Centres and specialist areas
Latest publication date: 16/05/2024
Supervising author: Dr Monsaert Els



