Ablation for atrial fibrillation
What is it?
What is it?Ablation is a treatment of certain heart rhythm disturbances. The rhythm disturbances often arise from a 'short circuit' in the heart's conductive tissue. Ablation can help eliminate this short circuit in the heart.
Ablation is often performed immediately following the electrophysiological examination. This treatment is particularly effective for most heart rhythm disturbances and is associated with few complications, which is why it is often preferred to treatment with medication.
What is the process?
What is the process?Preparation
Blood thinner medication is preferably started one month before the procedure, and the dose will be determined by the GP based on blood tests.
In preparation, a CT scan of your heart is performed. The CT scan allows the physician to make a 3D reconstruction of your heart, which will act as a guide during the procedure.
You will be admitted to the cardiology day hospital. You must be fasting on the day of admission: at least 2 hours for clear liquids (water, tea and coffee only), at least 6 hours for a light meal and dairy products, at least 8 hours for a normal meal. You may take your medication as agreed with the physician.
If no recent laboratory results are available, blood samples may be collected.
You will be given a surgical gown to wear. The nurse will place an IV line in your arm for the administration of medication, should that be necessary.
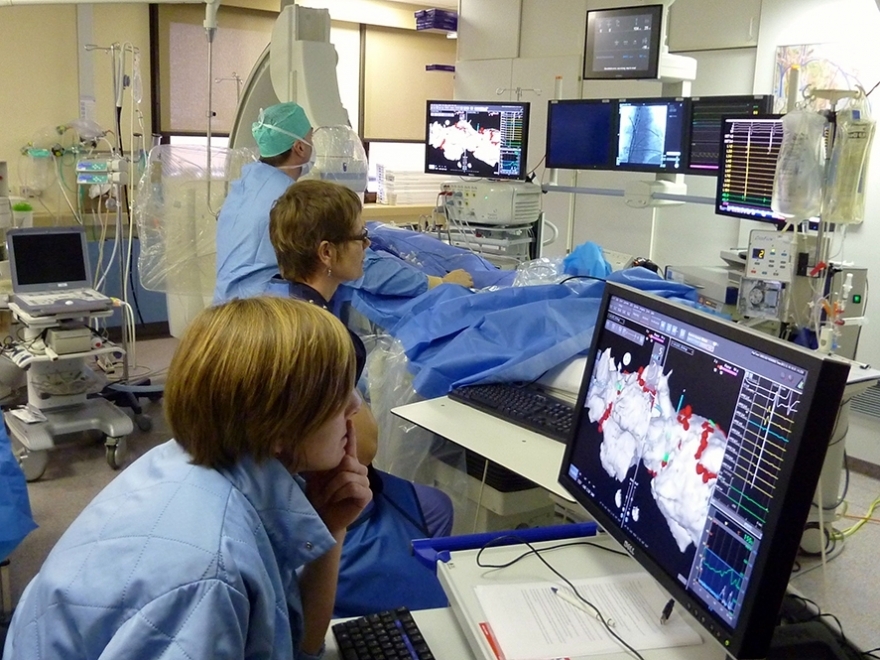
The procedure is performed in the cardiac catheterisation room.
Test
You take place on the examination table. Ten adhesive electrodes are placed to monitor your heart rhythm. Because the procedure may take a long time (2.5 hours) and it is extremely important that you remain still, you will receive a general anaesthetic for your comfort. Before the procedure starts, clots in the heart should be ruled out using oesophageal echocardiography. An area of skin measuring 5 by 5 cm is shaved and disinfected, and adhesive sterile sheets are placed around it. The vein and artery in the groin are pricked, providing access to electrical catheters that are directed into the heart. With the help of X-ray, the position of the catheters can be confirmed. With 1 or 2 transseptal punctures, catheters are inserted through the septum into the left atrium.
Using CARTO® imaging and the CT scan to provide a 3D view, the pulmonary veins are isolated from the rest of the heart through burns that are delivered with an ablation catheter. Other sensitive areas generating stimuli are also located and isolated. The rhythm disturbance disappears or the normal heart rate is re-established through cardioversion. After checking the result, the catheters are withdrawn. A compression bandage will be placed on the groin. You will wake up in the Cardiology Day Hospital. You will need to stay in the hospital for one night.
Aftercare
In order to prevent infection, it is recommended that you not bathe for the first two days (but you may shower). During the first week, heavy duty at work or physical exertion is not advisable.
What are the risks?
What are the risks?The procedures has a few risks. You may have bruising in the groin. This is best prevented by using a strong bandage and by lying flat.
In 0.5% of the procedures, bleeding can occur due to perforation of the heart wall causing the sac around your heart to fill with blood. This may disappear by itself, but sometimes intervention by a heart surgeon is necessary to close the perforation.
In 0.3% of cases there is a risk of embolism. For this reason, blood thinners are started in advance and kept at the right level around the time of the procedure. You will need to continue taking this medication for at least three months.
Results
ResultsTreatment is expected to be successful for 60-90% of patients. Of patients, 20% will require a second treatment for this.
The chance of establishing a permanent stable sinus rhythm depends on various factors. It is the highest in young patients who have short episodes of atrial fibrillation, who have no structural coronary heart disease and who had their first atrial fibrillation recently. The chance of permanent success decreases with age, with the duration of the arrhythmia episodes, with the degree of structural heart abnormalities and with the time since the first episode.
Leaflet
LeafletOnly available in Dutch:
Pulmonale venen isolatie (PVI)
DownloadCentres and specialist areas
Centres and specialist areas
Latest publication date: 16/05/2024
Supervising author: Dr Provenier Frank



