Specialised Nail Centre: a unique unit
Discoloured, thickened or crumbly nails are often attributed to mycosis by GP s and other physicians. In many cases this is the correct nail pathology, but the range of possible causes is much wider. At Maria Middelares General Hospital, nail abnormalities are given a special place in the specialised Nail Unit on the Dermatology Department.
Dermatologist Dr Linda Temmerman points at the increased importance of the subspecialty within dermatology, especially nail pathology: ‘In this way, we can achieve a more accurate diagnosis for a variety of conditions - from innocent to serious ones - and offer our patients better treatment with more comfort.’ Patients increasingly ask for advice about a nail that does not look right. The aesthetic aspect plays an important part in this, but a damaged nail can indicate an underlying pathology such as a (benign or malignant) tumour, inflammatory dermatosis, etcetera. Patients often come to the specialised Nail Unit at Maria Middelares General Hospital for treatment.
‘A damaged nail can indicate an underlying pathology such as a tumour, inflammatory dermatosis.’
Dr Veerle Dhondt has been involved in training and conferences on this subject for ten years already and is now an expert in the field. She explains: ‘It has become increasingly clear that additional experience in nail conditions really is necessary. It requires years of experience, specialised training and skills to become familiar with nail pathologies and especially with the specific surgical procedures. Many dermatologist colleagues refer patients to us because of our expertise.’ Maria Middelares General Hospital now has a specialised team that consists of three nail surgeons. Dr Veerle Dhondt has worked at Maria Middelares General Hospital since 2008 and has now become one of the main nail experts in Belgium. She is supported by Dr Jolien Veramme and Dr Sam Dekeyser who, as dermatologists, have also studied specific nail diseases. The team is completed by a specialised nurse who is skilled in conservative treatment.
Nail conditions - categories
1. Biopsies for diagnosis
Pigmentation changes, inflammatory diseases (psoriasis/lichen...), tumours
2. Surgical removal
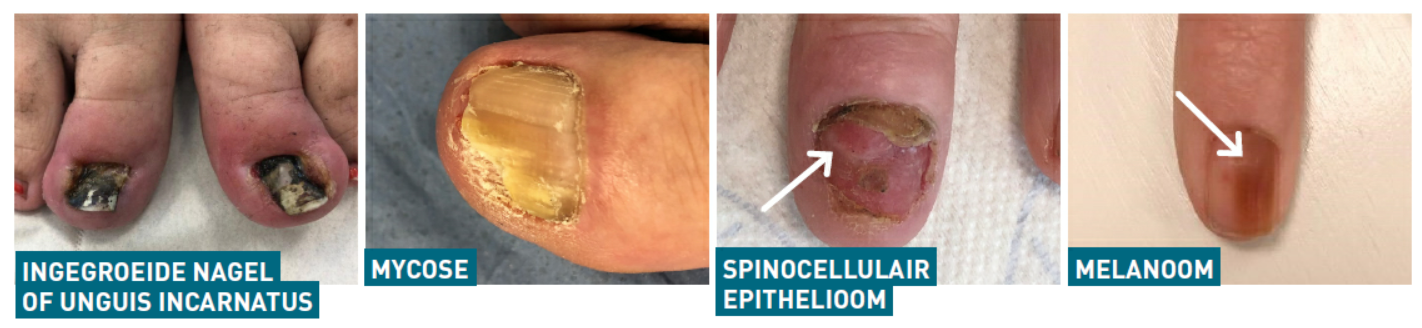
- Tumours (benign, malignant, precancerous conditions): mucoid cyst, periungual fibroids, fibrokeratomas, onychomatricoma, glomus tumour, exostoses, verrucae, botryomyncome, pre-cancers or cancers such as Bowen’s disease, spinocellular epithelioma, melanoma
- Ingrown nails with/without hypergranulation tissue, pincer nail, retronychia. Nails that have been clipped too short or too angled sometimes grow inward at the edge, causing pain or keloids. Excessive skin and the ingrown part of the nail often must be removed surgically. Partial destruction of the nail root allows the nail to grow straight again.
Different from a standard dermatologic surgical procedure, physicians use phenol to chemically destroy the nail root (‘phenolisation’). This means less post-operative pain, less risk of complications such as bone infection and less risk of recurrence.
Onychauxis versus nail fungus
- Onychauxis is a thickening and yellow discolouration of the nail plate, without an underlying infection. They may be the result of prior trauma or of reduced blood supply to the nails (e.g. in the case of arteriosclerosis in the legs, smoking, etcetera). Treatment consists of filing the nails and keeping them soft, but full recovery is often not possible.
- Nail fungus may also cause thickening of the nail plate, often with typical yellowish-brown discolouration and flaking under the nail plate. During the consultation with the physician or nurse, a large sample of it will be taken. Treatment is possible with prolonged ingestion (usually several months) of antifungal medication and mechanical removal (milling) of the remaining diseased fungal fragments.
Other infections (bacterial, yeast infections) can also infect the nail and the skin around it. Adequate and targeted cultivation is important to start the right treatment.
Serious conditions
If there is discolouration (red line, brown or black discolouration, etcetera) or splitting of the nail, if there are visible structural changes under the nail or if slimy fluid appears from under the nail when pressed, this may point to benign or malignant growths. A great many inflammatory dermatoses such as psoriasis, lichen planus or other auto-immune diseases such as alopecia areata can also be recognised from specific nail abnormalities. Additionally, we must not forget external factors such as soap, water and manipulations which may have an impact on the nails. A number of internal conditions or medications also result in specific abnormalities.
Too often the conclusion is a fungal infection and patients are randomly started on medication. It is therefore important to know that a permanent change to the nail is not always innocent, but may in fact have a serious underlying cause.
Practical information for nail procedures
- Procedures last 30 minutes on average. We ask you to arrive ten minutes in advance and wear or bring an open shoe (slipper, wide sandal). It is advisable to bring someone who can take you home afterwards.
- On the day of the procedure and the day after, the patient will not be able to work or go to school. It is also best not to plan any major activities on the weekend following the operation. The Monday after the operation, a normal shoe can be worn again in most cases.
- Post-operative wound care depends on the procedure. Usually the bandage remains in place for 48 hours. The treated area may then be soaked in a lukewarm footbath. Afterwards, care with an antiseptic is recommended.
- It is recommended to keep the foot up for the first 48 hours after surgery.
Contact
The secretariat of the Dermatology Department can be contacted on +32 (0)9 246 78 01 or +32 (0)9 383 69 08.
Online appointments are available too.


