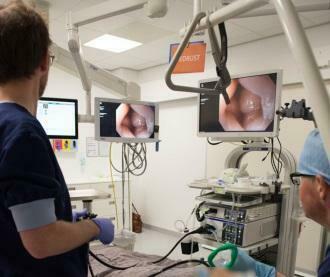
Maria Middelares General Hospital recognised for innovative treatment of oesophageal problems
Stomach acid may flow back into the oesophagus (known as ‘reflux’) if the valve between the stomach and the oesophagus does not close properly, for instance because of obesity. Long-term reflux may turn the mucous membrane in the lower part of the oesophagus into a pinkish kind of ileum mucous membrane, also known as Barrett’s oesophagus. Approximately one in ten of people with reflux complaints actually develops Barrett’s oesophagus. Over time, abnormalities may develop in the mucosa of Barrett's oesophagus, which may, again over time, evolve into cancer.
Cancer risk
In view of the risk of developing malignancies, patients with Barrett's oesophagus are monitored through regular gastroscopies with biopsies. If any abnormalities are found or if biopsies yield abnormal findings, the abnormality must be examined and removed. The technique that is used for this is endoscopic submucosal dissection (ESD). The gastroenterologist inserts an ultra-small knife and camera into the oesophagus through the throat. The surgeon then cuts out the abnormality entirely, without injuring the muscle. This means that the patient suffers minimum discomfort after the procedure. An additional advantage is that the tissue can be examined properly by a pathologist afterward. Earlier techniques often required the surgeon to remove the abnormality in pieces, complicating any analysis.
Because ESD is a complex technique that requires high skill levels and is associated with higher risk if the level of experience with the technique is insufficient, ESD is only performed on a regular basis by a handful of endoscopists in Flanders.
Preventing recurrence
Patients who develop a malignancy or a precursor are at high risk of developing a recurrent abnormality in a different location (metachronous lesion) in the Barrett's mucosa. To effectively reduce this risk, Barrett's oesophagus is treated by means of the RFA method.
Dr Pieter Dewint (interventional endoscopist): ‘During RFA, the “bad” mucosa is very carefully removed by briefly applying intense heat to this layer of the oesophagus, thus destroying it. The gastroenterologist performs this procedure during a gastroendoscopy. After the procedure, the oesophagus heals and the oesophagus’ original protective layer grows back.
The RFA technique is also only offered in a limited number of large hospitals. The Digestive Centre at Maria Middelares General Hospital has been one of these since 1 April 2018.
Dr Ronny Goethals (medical director): ‘Through the expertise of our interventional endoscopist, we have the knowledge and skill to be able to apply both endoscopy techniques (ESD and RFA) swiftly and safely. Dr Dewint is supported by a multidisciplinary team of gastroenterologists, oncologists, pathologists, radiologists and surgeons at Maria Middelares General Hospital.’
Reimbursement
The current reimbursement criteria indicate that, to qualify for reimbursement, a patient must have an increased risk of developing a malignant tumour in the Barrett's mucous membrane. This is a good rule since the treatment is relatively expensive and because – as always – any medical procedure is associated with side effects.
Reimbursement criteria are as follows:
- early stage oesophageal cancer that was removed by a gastroenterologist;
- biopsies or abnormalities in the oesophagus indicating high-grade dysplasia, i.e. the pre-cancerous stage.